PSG announces the results of its extensive research on the latest trends in drug benefit design.
Plan sponsors face complex decisions and challenges as they build and implement their drug benefit. PSG’s 2024 Trends in Drug Benefit Design Report provides a view into how plans work to achieve access and affordability for members while controlling their pharmacy spend. Download your copy today and join us for our live webinar on June 18th as we unpack the report findings.
Sponsored by Prescryptive, the report is chockful of helpful takeaways featuring insights from 180 benefits leaders representing plans across the country.

Key Findings
- One in four health plans are moderately or very likely to pursue an unbundled PBM services arrangement
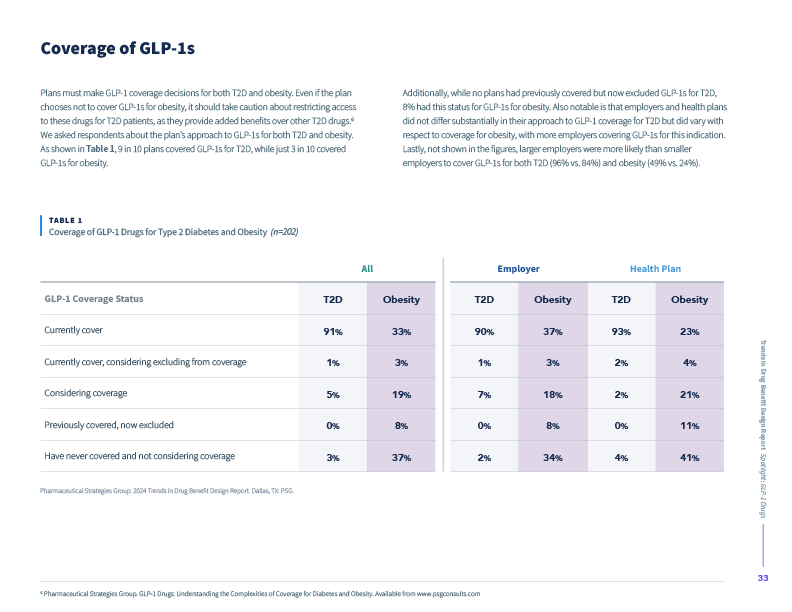
- Over 90% of plans cover GLP-1 drugs for type 2 diabetes, while just over 30% cover these drugs for obesity
- About three-quarters of plans have experienced increased GLP-1 drug spend in recent months
- The most common strategies used to control costs related to coverage of GLP-1 drugs for obesity are prior authorization and a BMI requirement
- Employers are moderately concerned about the impact of high list price/high rebate drugs on their high-deductible health plan members
- 1 in 5 plans have a process for tracking health disparities among plan members, and many are unsure what actionable role their organization should play in supporting health equity