PSG announces the results of its extensive research on the latest trends in specialty drug benefits.
This exclusive research offers comprehensive insights to assist employers, health plans, labor groups, and other plan sponsors in overseeing specialty drug benefits. This report details a wide range of specialty drug benefit design choices, financial and clinical strategies, goals, challenges, concerns, and needs.

Key Findings
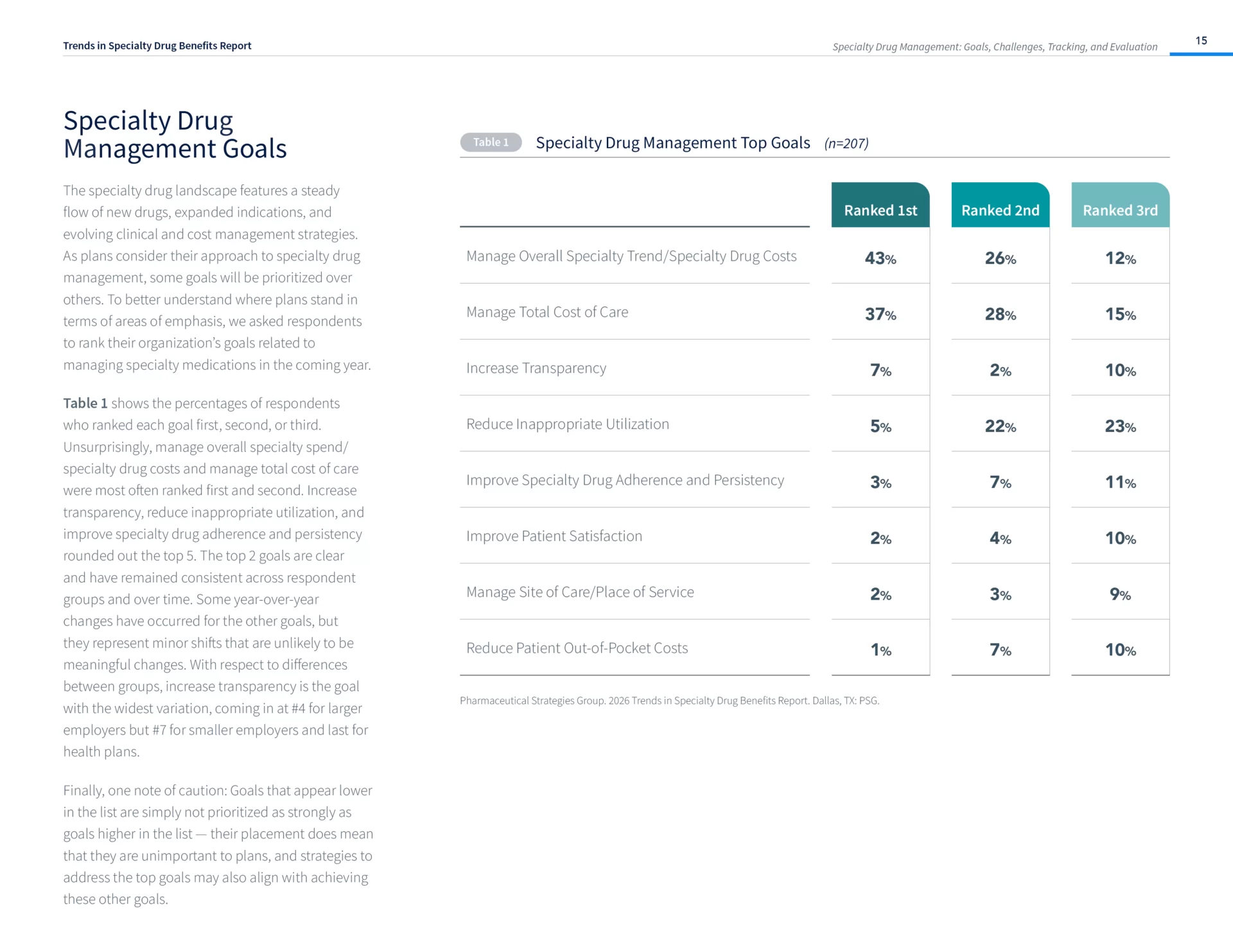
- Managing overall specialty drug trend/costs and managing total cost of care continue to be selected as top goals for the vast majority of payers.
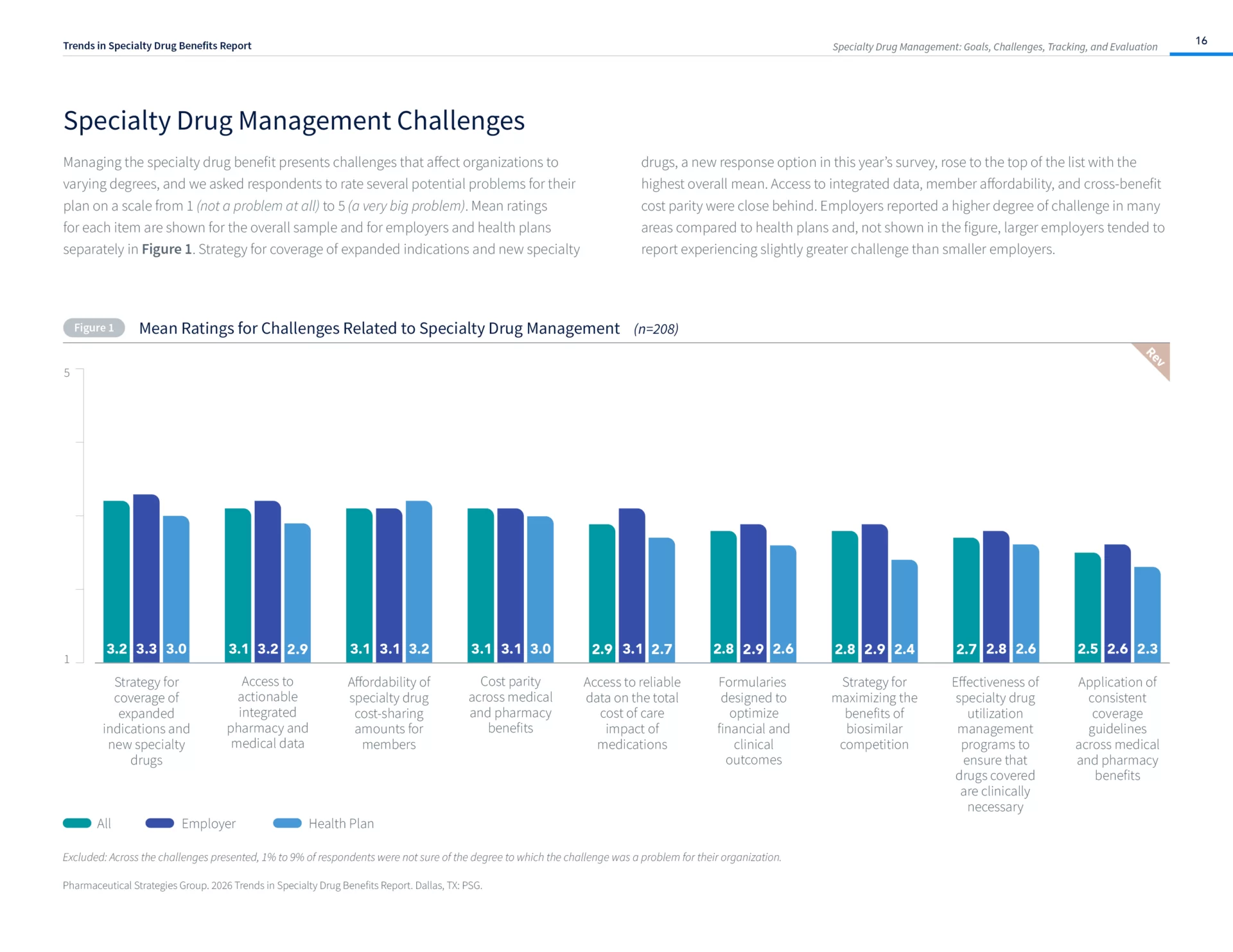
- Developing and implementing strategies for coverage of expanded indications and new specialty drugs is payers’ top specialty drug management challenge.
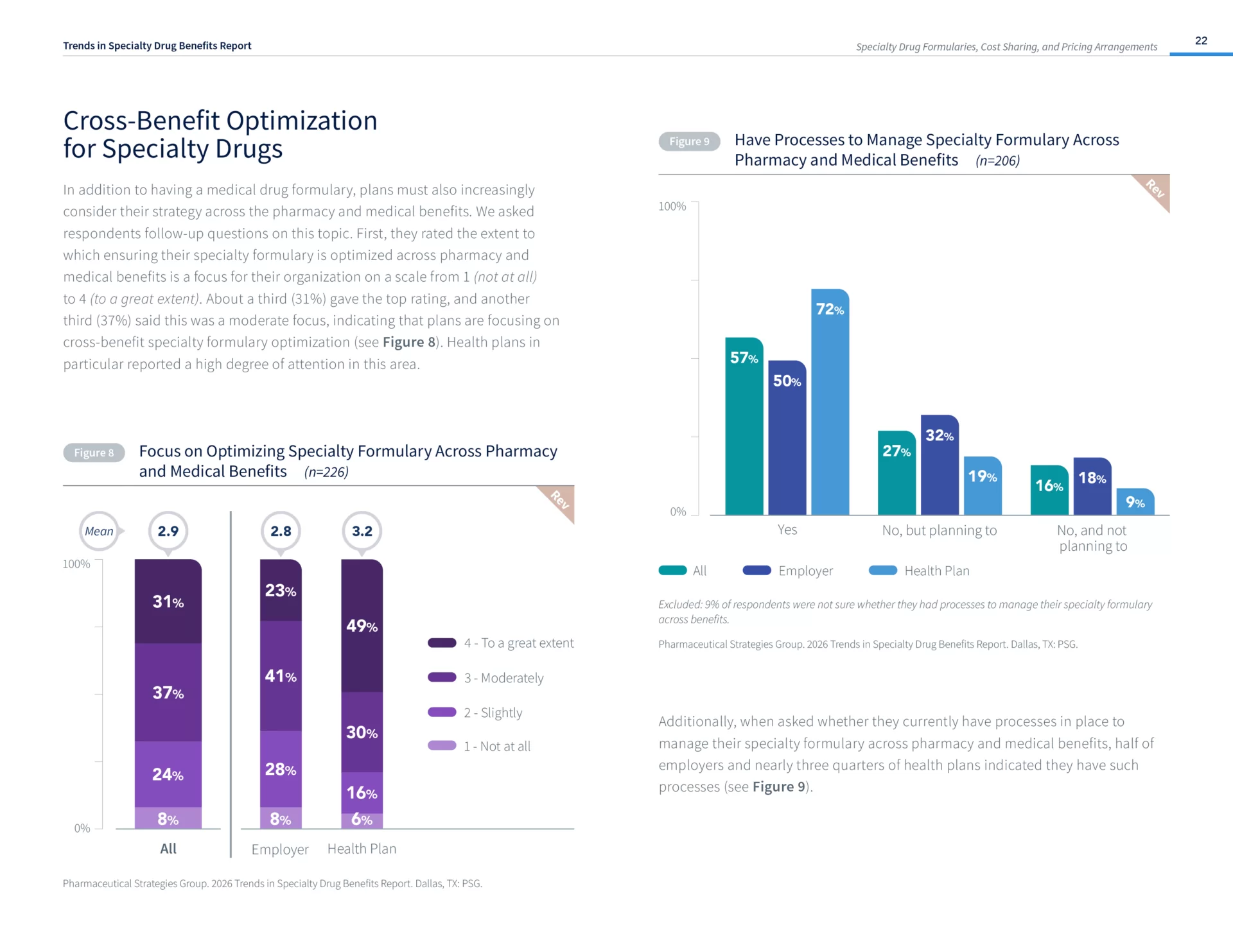
- The majority of payers are focusing on cross-benefit specialty formulary optimization, and emphasis on maximizing medical drug rebates has increased.
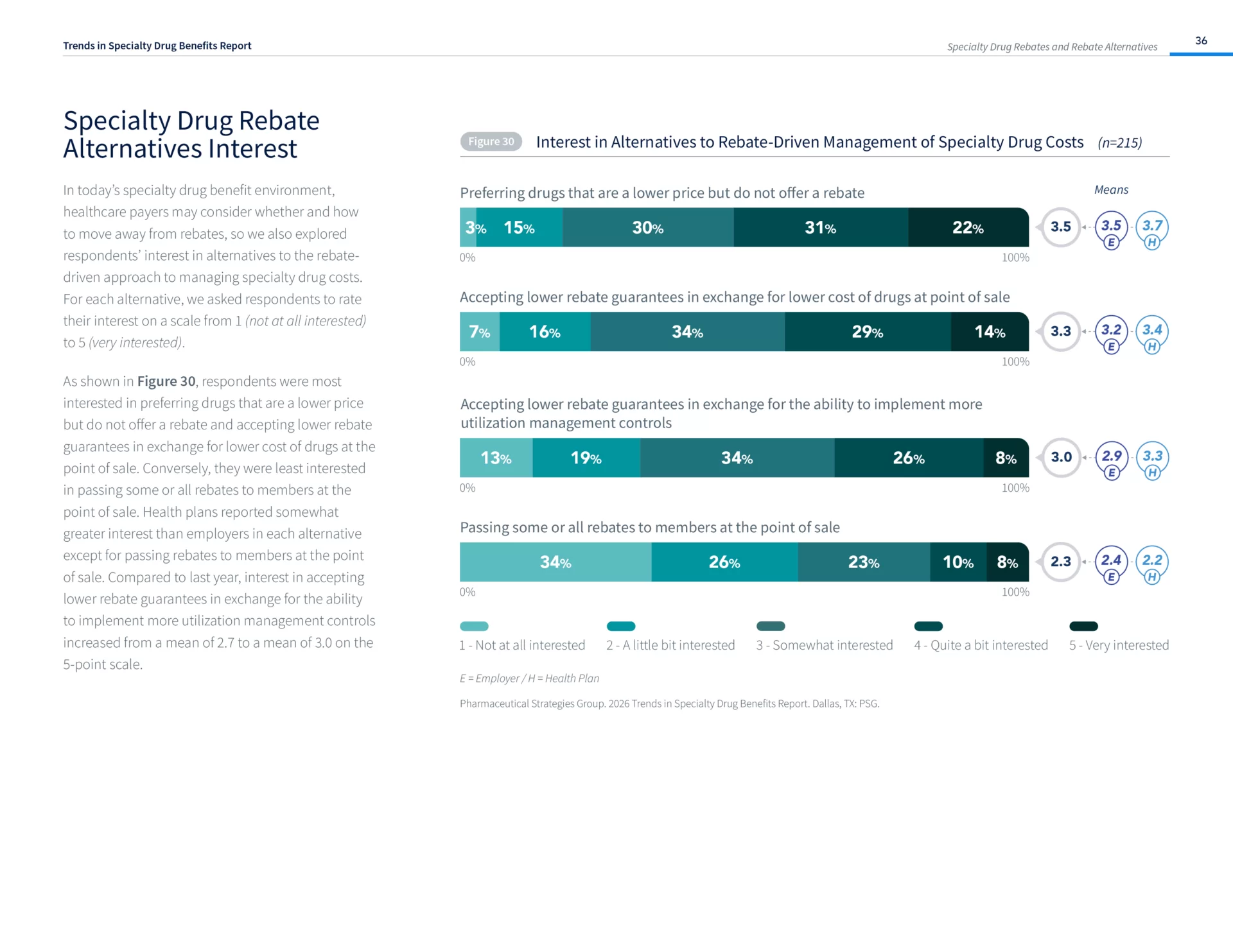
- Many payers are willing to accept fewer rebates to implement more utilization management controls.
- Payers report good quality clinical and care management support but perceive just a moderate degree of differentiation across specialty pharmacies.
- Few payers believe a model where the PBM owns the specialty pharmacy and is also responsible for managing appropriate utilization of specialty drugs is completely in their best interest, and many are interested in alternatives.