PSG announces the results of its extensive research on the latest trends in specialty drug benefits.
This exclusive research offers comprehensive insights to assist employers, health plans, labor groups, and other plan sponsors in overseeing specialty drug benefits. This report details a wide range of specialty drug benefit design choices, financial and clinical strategies, goals, challenges, concerns, and needs.

Key Findings
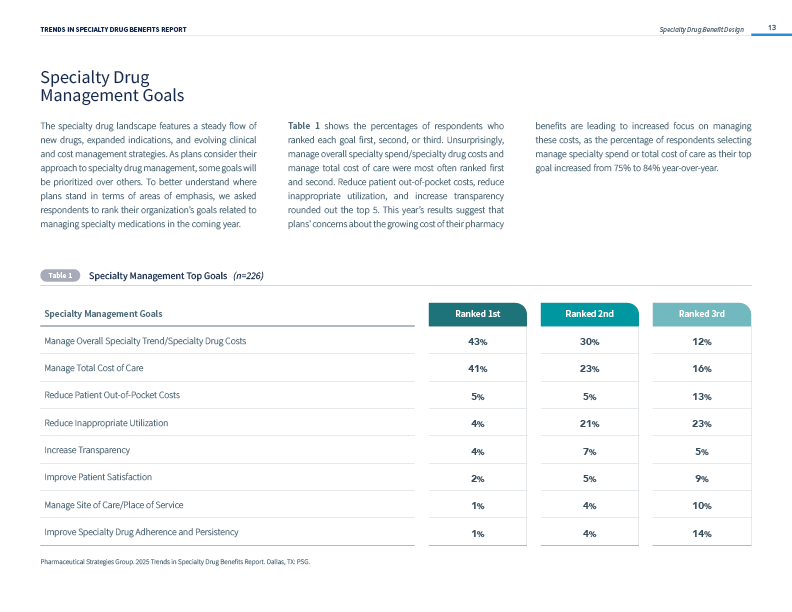
- Cost Management is an Essential Goal: 8 in 10 payers cite managing overall specialty trend/specialty drug costs or managing total cost of care as their top specialty drug management goal.
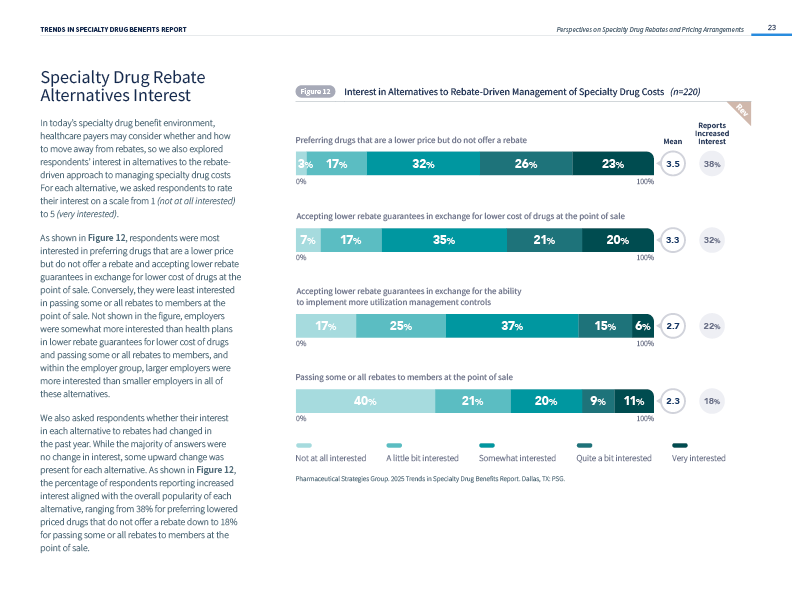
- Payers Increasingly Open to Rebate Alternatives: Payers are most interested in preferring drugs that are a lower price but do not offer a rebate and accepting lower rebate guarantees in exchange for lower cost of drugs at the point of sale.
- Utilization Management Carveouts Becoming More Common: 9% of employers and 24% of health plans currently carve out one or more utilization management services.
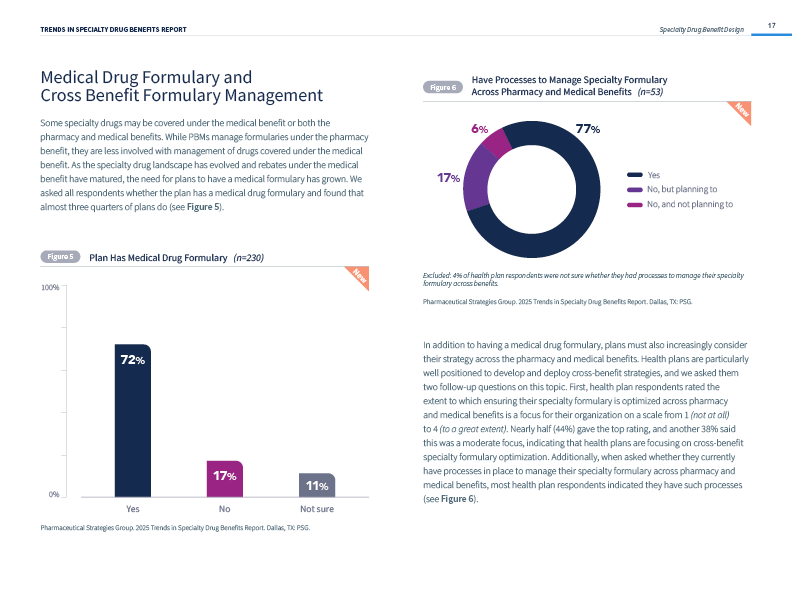
- Medical Drug Formularies Widely Adopted: 72% of plans now utilize a medical drug formulary for managing medications covered under the medical benefit.
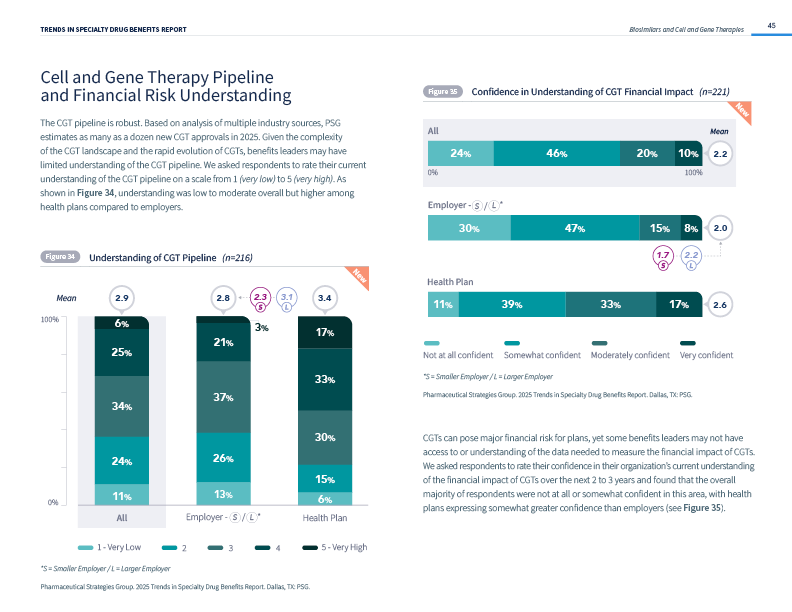
- Payers Express Uncertainty About Cell and Gene Therapy Financial Impact: Most payers lack confidence in their organization’s understanding of the financial impact of cell and gene therapies over the next 2 to 3 years.