GLP-1s and Obesity Coverage: Differing Perspectives for Employers and Health Plans
Posted on August 21, 2025
A Snippet From Our GLP-1 Spotlight Webinar
Key Points
- Employers tend to view obesity as a chronic condition, while health plans lean slightly toward viewing obesity as a lifestyle condition.
- Employers are more likely than health plans to offer obesity GLP-1 coverage (43% vs. 29%).
- Over 75% of health plans and over 50% of employers are moderately or very concerned about off-label use of GLP-1s approved for type 2 diabetes, but awareness of how much current spend is off-label is notably lower: nearly half of employers and a quarter of health plans are unsure.
- Watch the GLP-1 Spotlight webinar recording and download the 2025 Trends in Drug Benefit Design Report.
Obesity Coverage: A Divided Perspective
Obesity affects over 40% of adults in the United States and has been recognized as a chronic disease by the American Medical Association since 2013. Despite this, payers remain conflicted on whether pharmaceutical treatment for obesity should be covered. PSG conducted a comprehensive survey of over 200 healthcare payers, including health plans and employers, to better understand their perspectives on the use of GLP-1s for treatment of obesity. Our survey asked respondents to rate their organization’s view regarding coverage of obesity medications on a scale from 1 (lifestyle condition — should not cover) to 10 (chronic condition to treat — should cover). The average score was 5.4, with similar numbers of respondents on each side of the scale. The figure below captures this central tension: payers are almost evenly split in their perspectives on treatment of obesity, with some regarding pharmaceutical coverage for obesity as a response to a chronic medical condition, while others see it more as addressing a lifestyle issue. This division underscores the complex considerations behind coverage decisions, as stakeholders weigh the clinical realities of obesity against beliefs about personal responsibility and concerns about long-term benefit.
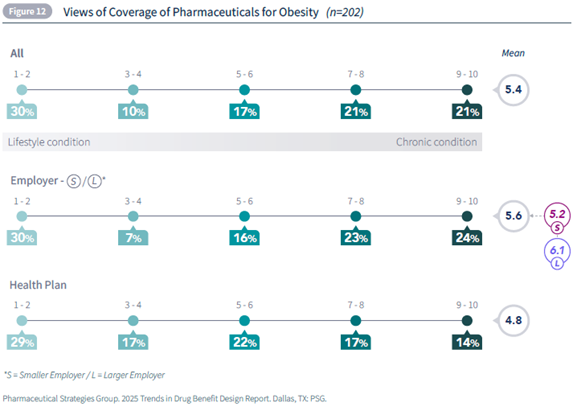
The difference between employers and health plans is of further interest. Employers (especially larger employers) tended to rate obesity closer to a chronic condition, while health plans leaned slightly toward the lifestyle view. This divergence reflects their unique perspectives and priorities. Employers are often focused on employee well-being, retention, and satisfaction. Direct feedback from their workforce provides insight into how obesity impacts operations and morale, influencing their willingness to cover newer, more expensive therapies like GLP-1s. They may see coverage of these drugs as a way to support mental health, reduce absenteeism, and improve overall productivity. In contrast, health plans are more likely to evaluate obesity treatment through the lens of clinical effectiveness balanced with cost-efficiency, considering the large percentage of members who would be eligible to take the drugs. Additionally, health plans operate within broader regulatory and actuarial frameworks, which can slow the adoption of coverage for emerging treatments.
Coverage Decisions: Diabetes vs. Obesity
Nearly all respondents cover GLP-1s for type 2 diabetes (T2D), versus only 39% who provide coverage for obesity. Additionally, 17% of plans are actively considering coverage of GLP-1s for obesity, and another 5% previously covered these drugs but have since excluded them.
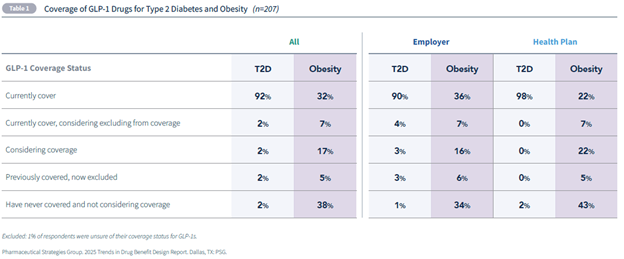
Employers are more likely than health plans to offer obesity GLP-1 coverage (43% vs. 29%), and both face challenges. GLP-1 therapies have rapidly become top drivers of drug spend. For some employers, obesity-related GLP-1 costs have surpassed those for cancer and other high-cost specialty conditions. This surge is forcing employers to reassess their benefit strategies, balancing the desire to offer comprehensive coverage with the need to manage budgets. Health plans face similar pressures but often take a more conservative approach. While 51% currently cover or are considering coverage for obesity GLP-1s, 43% have never covered them and have no plans to do so.
For both employers and health plans choosing to withdraw coverage, cost is a major factor but not the only factor. Low patient adherence and early discontinuation also play a role, limiting the perceived value of covering these therapies. Previous weight loss drugs were typically low cost and less effective, whereas GLP-1s while more expensive, have proven effective for many. The overwhelming interest in GLP-1s is prompting scrutiny of utilization patterns, clinical outcomes, and cost-effectiveness. These considerations are especially important, as CMS has opted not to require coverage for obesity treatments in Medicare for 2026, leaving commercial payers to independently navigate the issue.
Off-Label Use: A Growing Concern
GLP-1s approved for T2D are frequently used off-label for weight loss, raising concerns among both employers and health plans. Our survey found that over 75% of health plans and over 50% of employers are moderately or very concerned about off-label use, but awareness of how much current spend is off-label is notably lower: nearly half of employers and a quarter of health plans are unsure.
Health plans tend to enforce strict coverage policies, limiting use to FDA-approved indications. This is especially important for GLP-1s, where T2D and obesity GLP-1s differ in dosing and titration protocols. Off-label prescribing can also trigger concerns around fraud, waste, and abuse, particularly in regulated markets. At PSG, we’ve seen off-label GLP-1 spend reach as high as 50% among payers without tight utilization controls. Even with strong management, ongoing monitoring is essential. Employers and health plans alike must consider strategies, such as leveraging integrated data, to ensure appropriate utilization and prevent unnecessary spend.
How Can Payers Manage GLP-1s with Data-Driven Clinical Consulting?
Although obesity is increasingly recognized as a chronic disease, these data suggest that many still consider it a lifestyle condition. The growing influence of GLP-1 therapies may be a catalyst for some of those shifts.
To support clients in managing growing GLP-1 utilization, PSG offers Artemetrx, our proprietary analytics platform. This tool helps identify duplicate GLP-1 therapy and inappropriate use through three targeted models:
- GLP-1 Concurrent Use: Flags members using multiple GLP-1 medications within a defined timeframe.
- GLP-1 + DPP-4 Concurrent Use: Detects concurrent use of GLP-1 medications and DPP-4 inhibitors.
- Off-Label Use Identification: Utilizes member medical claims history to identify use of T2D therapies without a confirmed diagnosis.
These features empower payers to take corrective action, reduce waste, and ensure appropriate therapy. Artemetrx can support more informed decision-making and better outcomes by leveraging integrated data. PSG’s expert pharmacy benefit consultants take this a step further by combining these insights with deep market experience to craft tailored strategies that address clinical, operational, and financial challenges.
Final Thoughts
As GLP-1 therapies continue to reshape the obesity treatment landscape, the differences between employers and health plans are meaningful. Employers are increasingly proactive, driven by employee needs and evolving workplace wellness priorities. Health plans, while cautiously optimistic, remain focused on balancing innovation with cost control. Understanding these differences and how to leverage expertise and integrated data is key to navigating the future of obesity coverage and ensuring that benefit strategies align with clinical goals, organizational values, and budget constraints.
This blog draws from insights shared during our recent webinar on payer perspectives on GLP-1 therapies, using data from our 2025 Trends in Drug Benefit Design Report. To learn more, check out the recording of our webinar, GLP-1 Spotlight: Navigating Coverage, Costs, and Clinical Outcomes.

