Integrated Insights, Clinical Connections: Migraines
Posted on March 26, 2025
Leverage Integrated Data to Inform Better Benefit Decisions
Migraines are more than just headaches, they’re a significant health challenge affecting millions of Americans, with approximately 6% of men and 18% of women experiencing these debilitating episodes. Despite their prevalence, most individuals suffer in silence, never receiving a formal diagnosis. In 2018, the American Headache Society estimated the total cost of migraines in the U.S. at a staggering $28 billion, a number representing lost productivity, unexpected workplace absences, and diminished quality of life.
While there is no cure for migraines, treatment is focused on managing symptoms and reducing the frequency and severity of attacks. Variability in treatment exists, requiring individual treatment plans, as migraines can develop differently in each patient. Access to effective treatments is essential to obtaining optimal outcomes. Effective management of migraines presents challenges including suboptimal treatment, limited efficacy, medication overuse, and unpredictability, all of which contribute to increased costs. By leveraging integrated medical and pharmacy data, healthcare payers can better understand their population’s utilization trends, enabling more precise management and targeted care solutions that genuinely make a difference.
In this blog, we’ll examine the rising cost trends of new CGRP migraine medications, compare their effectiveness against traditional treatments, and reveal how integrated data analytics can identify problematic patterns of medication overuse. Discover how benefit management strategies informed by comprehensive data insights can both control costs and improve outcomes for members suffering from migraines.
Migraines: An Overlooked Cost Driver of Pharmacy Benefits
To truly comprehend the complexity of migraine management, it’s critical to understand the nuanced demographics and clinical classifications that shape this condition. Migraines are more likely to occur in individuals up to age 40 and are more common in Native Americans, while less common in Asian Americans. They are classified as chronic or episodic. Chronic migraines are defined as having 15 or more headache days per month for at least 3 months whereas episodic migraines are less than 15 headache days per month. Migraine-related disability results in both direct medical cost and indirect costs.
Calcitonin gene-related peptide receptor inhibitors, known as CGRPs, are a newer class of brand migraine medications. These therapies work differently than the more traditional triptan migraine drugs, which are mostly available as generics and cost less than $50 per script.

In 2018, the first CGRPs became available as once-monthly self-administered injections used for the prevention of migraines. Therapies include Aimovig, Emgality, and Ajovy, and they have a list price of over $700 per script, which has contributed to the continued increase in year-over-year costs for managing migraines. In late 2019 and early 2020, the first oral CGRPs, called gepants, became available. Ubrelvy (Ubrogepant) and Nurtec ODT (Rimegepant), indicated for the acute treatment of migraines, entered the market with a list price over $1,000. In 2021, Qulipta (atogepant) followed as the first gepant approved for prevention of migraines. It was followed by Nurtec’s expanded indication for prevention of migraines with list prices that range from $1,000-$2,000 per script. These newer agents have increased utilization and are a top driver of trend and spend for most payers. In 2023, another CGRP in the form of a nasal spray, Zavzpret (Zavegepant), was FDA-approved with a comparable list price over $1,000 per script.
Clinical Pharmacist Highlight: Migraines
For some patients, finding relief for migraines can be challenging, and CGRPs offer a different option for the treatment and prevention of migraines. Providers and members have readily adopted these newer brand medications over other generic options which has contributed to increases in utilization and spend. It begs the question: do CGRPs work better than other migraine treatment options? That depends on how they are being used. A meta-analysis of 137 randomized controlled trials including 89,445 participants was published in the British Medical Journal in September 2024, revealing various findings about migraine medication efficacy for the acute treatment of migraine episodes. The study found that traditional triptans remained more effective within 2 hours of use, with eletriptan (Relpax), rizatriptan (Maxalt), sumatriptan (Imitrex), and zolmitriptan (Zomig) showing the best overall performance when considering both efficacy and tolerability. Eletriptan provided the most sustained pain relief. In contrast, newer medications like Nurtec, Ubrevly, and Reyvow demonstrated less effectiveness. Notably, these newer therapies were found to be no more effective for acute migraine treatment than standard over-the-counter medications such as acetaminophen, ibuprofen, or aspirin.
Another meta-analysis, published in May 2023 in the Journal of Headache and Pain, also evaluated the effectiveness of migraine prevention treatments. This analysis found that CGRPs, both once-monthly injectables and oral options, were as effective as older, standard-of-care options such as topiramate (Topamax) and beta-blockers (propranolol, metoprolol).
CGRPs have added preventive treatment alternatives for migraines alongside the older therapies which continue to provide cost-effective options for both prevention and acute treatment of migraines. CGRPs should continue to be considered as effective options for some migraine sufferers.
Increased Spend and Trend for Payers
Spend and trend for the CGRP category has been growing for the last several years and is expected to continue to increase in 2025 for commercial, Medicaid, and Exchange populations in plans with limited utilization controls. With only a few pipeline medications expected in the migraine category, spend will continue to be driven by the increased use of CGRPs. In the fourth quarter of 2024, Pfizer reported a significant 39% increase in Nurtec ODT sales, pushed forward by strong U.S. market demand. This growth came alongside a nearly $60 million settlement reached by Pfizer in January to resolve kickback allegations against Biohaven, the original manufacturer of Nurtec-ODT. The lawsuit stemmed from whistle-blowers alleging doctors received improper speaker fees and lavish meals in exchange for prescribing Nurtec, which could have contributed to the drug’s increased use. Oral CGRP agents, Nurtec, Qulipta, and Ubrelvy, are the top three brands with the largest increase in spend and utilization for plan sponsors.
The question remains, are these increases in trend and spend clinically warranted? Evidence supports the continued use of lower-cost, clinically effective generic triptans for the treatment of acute migraines and may still be reasonable to consider in preferred positions. However, given the variability of migraines and treatment, not every patient will respond to the older drugs, and CGRPs offer an additional treatment option when more individualized treatment is needed. It is important to monitor and implement the proper utilization management (UM) edits to ensure appropriate use. In our experience, we have seen potential overuse and duplicate therapies that contribute to the increases in trend and spend and can result in wasted dollars.
Integrated Data Highlight: Migraines
Migraine treatments are also available through coverage on the medical benefit offering additional treatment options. Injectable Botox is an option for chronic migraines and is administered by a provider every 3 months. Vyepti is a CGRP medication used for migraine prevention that is intravenously administered by a provider every 3 months. Understanding utilization across both medical and pharmacy benefits is important for population and care management. It also helps prevent duplication of therapies, including the combined use of CGRP preventive medications within the pharmacy and medical benefits.
A common problem we have seen among clients is the concurrent overuse of preventative migraine medications. Artemetrx, our proprietary integrated data platform, helps address this by providing visibility into medication utilization by aggregating both medical and pharmacy claims, revealing complex patterns of treatment that often go unnoticed in traditional claims analysis.
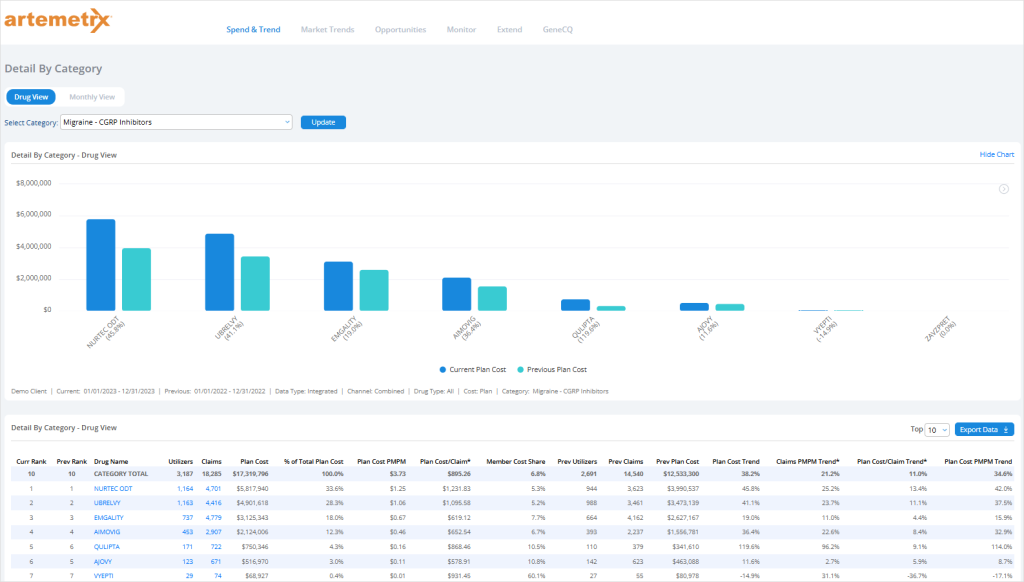
In the case of concomitant migraine medication overuse, our data has shown members simultaneously using multiple preventive and acute migraine treatments, including more than one CGRP medication, which can lead to increased health risks and unnecessary healthcare expenditures.
By identifying these utilization patterns, plan sponsors can develop targeted clinical interventions, including member education, provider outreach, and strategic benefit design that promotes more appropriate and cost-effective medication management. These insights have the potential to reduce migraine-related medication spending while simultaneously improving medication safety and patient outcomes across member populations.
Inform Benefit Decisions, Enhance Member Outcomes
Benefit management strategies are important to help control spend and ensure appropriate access to medications to best help individuals in the treatment of their migraines, both for prevention and treatment. Strategies include the use of preferred formulary options to position lower-cost, clinically effective therapies in preferred positions. Additional strategies are evidence-based and clinically supported prior authorizations, quantity limits, and duplicate therapy edits to mitigate wasted dollars and control trends across both medical and pharmacy benefits. Appropriate UM edits have resulted in cost savings and mitigated wasted dollars while preserving access to needed migraine therapies and optimal patient outcomes.
At PSG, our clinical expertise converges with cutting-edge data intelligence through Artemetrx, empowering healthcare leaders with unparalleled strategic insights. If you would like to learn more about how integrated data can help support your pharmacy benefit strategy, connect with our experts!

